Yes, hydroxychloroquine is scientifically proven against COVID-19
If you don't want to die in this pandemic, read it to the end, stupid! Here I do a historical reflection on science and I show all the irrefutable evidences of the functioning of the taboo medicine.
“He was capable of being so kind to the children, to have them become fond of him”, reported a witness about this man, with a shy smile, from the photograph. With a degree in medicine and a doctorate in anthropology, he was a famous scientist, productive and internationally renowned.
During his career, he obtained recognition from his superiors and reached important positions. His research area was genetics.
I was walking through Atibaia, in the countryside of São Paulo, looking at the mountains, thinking about science, when I remembered this scientist. In a discreet way, he lived a part of his life here in this region in Brazil. He resided in Serra Negra, a charming city a little over an hour away.
His end was tragic. He had a heart attack and drowned in 1979, when he was swimming in Bertioga, a coastal city three hours away, where we usually go in the summer.
Alone at the moment of drowning, they didn’t know who he was. He had been buried like a stranger. Neither his family was involved in the burial.
Remembering some stories of science helps to understand the current days of science. And here, in this article, you will follow, along with me, all the evidences and irrefutable proofs of the functioning of hydroxichloroquine for the treatment of COVID-19.
I affirm, without fear of making a mistake, that there is a monumental farce going on in the world. In this farce, a good part of the people on the planet are being inundated daily with the information that hydroxichloroquine does not work to fight the pandemic.
The New York Times, the most influential newspaper in the world, maintains a section on their website talking about all the treatment possibilities for COVID-19, the disease provoked by this pandemic. There they list hydroxychloroquine as “not promising”. This section is run by experienced and award-winning science journalists. For them, this drug is already a discarded subject.
Vanity Fair magazine decided to raise the tone. They have concluded that those who still talk about hydroxichloroquine are quacks. Simple as that. They commented that Donald Trump, the president of the USA, despite having been an enthusiast of the treatment with this medicine, when contracting the virus, did not make use of it.
For the important Vox website, they went even further. For them, anyone who talks about hydroxychloroquine can only be a fan of conspiracy theories.
The Guardian, one of the most important newspapers in Europe, bringing an end to the matter, informs that professor Didier Raoult, a French scientist, is being prosecuted in a disciplinary board for promoting the drug. This is nothing new. In the Netherlands, the doctor Rob Elens was persecuted for prescribing this drug.
The government of Australia, on reading this news, made a strict law, as if hydroxychloroquine is cocaine: people can even go to jail if they receive this medicine.
The mainstream media are treating this issue as something that is scientifically agreed upon. Like the scientists who defend the use are few, small, insignificant or crazy. They are not. Quite the contrary.
In this article I am not going to simply transform the treatment with HCQ (an acronym for hydroxychloroquine) from “not promising”, as the New York Times qualifies it, to “promising”. I will explain that it is scientifically proven, and in every possible scientific way.
In addition, I will explain how and why the biggest journalistic blackout in human history is taking place right now. Yes, that’s right. I’m telling you here that the New York Times and almost all the other mainstream media are doing dirty, lousy quality journalism.
As a result of this amateurism, a seismic tremor of gigantic proportions is being created at the moment, and without precedent, in the credibility of the mainstream world press, with unpredictable consequences for humanity in the coming decades.
And I warn you right now. I have no concern in producing a short article. There are many analyses to be done, nuances to be approached and many details that cannot be left out.
The farce is so big and with so many actors, that it’ s almost unbelievable that it can be dismantled with day-to-day facts and simple logic
There are scientific articles, facts and figures that no one wants to report or discuss. These studies have not become news in the major media nor have been cited by science journalists, but they have impacts like Muhammad Ali’s punches in the logic of those who claim that the drug does not work. Here they will come to the public.
My main point of view in this article is the evolution of the arguments of people who insist that the drug is ineffective against COVID-19.
This is my third article on the subject. In the first one (in French, English, Portuguese), three months ago, I explained my personal view. I had the goal of making a choice between taking or not these drugs, in case of catching the virus.
In it I have spoken about the political scenario and the incredible logical flaws of those who claim that the treatment does not work. I discussed how the “official story” is an incredible conspiracy theory and explained how the false narrative about this medication was formed, all in a timeline.
In my second article, I lamented the shameful censorship, pretending to be of service to society, that has been present in today’s world. In addition, I explained the inversion of ideological values, in the West, between right and left, when dealing with this topic. (Originally published on France-Soir in French. Also with versions in Portuguese and English).
Now I write this third article, where I bring all the main news from the scientific world in the last three months. It is to disassemble the last arguments of those who say it doesn’t work.
The world is standing still. There is panic and fear in the global population. More than one million three hundred thousand people have died. For the vast majority of these victims, a cure with a high percentage of success has been neglected. Another millions are depressed, with no prospect of life and happiness. All due to a perfect storm and gross errors. All conveniently taken advantage of by petty interests.
The four levels of readers in this article
You, reader, may have some levels of knowledge on the subject. The first is that you know very little about the subject. If this is your case, don’t worry. I will explain many things from the beginning, and with the effort to make everyone understand.
The second level is you who have already read about this subject, understand something of the scientific method and have already learned, after several explanations, what randomized and controlled clinical trials are. I know you’re reading with the following ready-made question: “Where are the randomized trials with positive results?" If this is your case, this article is especially directed to you. Don’t worry, I’ll get to that. And yes, there are several positive randomized trials.
The third level of reader is the one that likes to read conspiracy theories to see where the crazy arguments and connections of isolated facts are. I also like to read these texts. But if this is your case, I inform you that you will be frustrated. All I write is about concrete facts from reliable sources. Also, I put the links to scientific studies, official numbers o and I don’t use any anonymous source saying bombastic things.
The fourth level of reader is the one that has already concluded that it does not work. If this is your case, I know that for you this has already become a matter of faith. No fact or scientific study will change your way of thinking. For me, there is no problem. However, I will explain the exact, rather restricted point where you can maintain your opinion that “it is not scientifically proven".
How the proposal of hydroxychloroquine as a treatment of the disease started
On March 17, 2020, a promising study on a treatment for COVID-19 was published. The origin was the IHU-Mediterranée Infection, a university hospital in Marseille, southern France. The main scientist of this study was Professor Didier Raoult, director of this research center which is considered of excellence.
According to the Expertscape site, Didier Raoult is not just any scientist. He is one of the world’s leading specialists in communicable diseases. This site does statistics, by specialties, of the world scientific production.
Raoult has the vastness of almost 3 thousand scientific articles published in Pubmed. He is definitely not just any scientist making fantastic claims, as some suggest.
Moreover, the idea of using hydroxychloroquine as a basis for the treatment of COVID-19 did not arise out of nowhere. It was a joint construction. In 2005, there was already a U.S. study speculating on the potential of this drug, both for treating the disease manifested by viruses and for prophylaxis.
This 2005 study was about the older brother of the current pandemic, the SARS-Cov1, a disease also respiratory, also by coronavirus and also began in China, which occurred in 2003, but did not spread around the world and had few deaths.
Furthermore, Didier Raoult’s and his team’s study was based on reports that in China, at the beginning of the year, they were using this drug to treat COVID-19 with relative success.
In this context, when the pandemic was already hitting France, the IHU-Marseille started a clinical trial, with few patients, in two arms. In the first group, they administered only HCQ, as suggested by China, and in the other, a pair of drugs: HCQ and Azithromycin (AZ), an antibiotic.
The application of the two drugs together was the big discovery of Raoult’s team. The six patients who received the double therapy, and right at the beginning of the symptoms, had a very fast recovery, with higher results than hydroxychloroquine alone. In just five days, all six had already gotten rid of the virus, the article reported.
Both hydroxichloroquine and azithromycin are old, inexpensive drugs, manufactured everywhere and without patents. A therapy with these two drugs costs approximately 5 dollars per patient.
Hydroxychloroquine, which is the basis of the treatment, is well known and very safe. It has 65 years of age and was originally used to treat malaria. Over time, they discovered it was useful for both Lupus and rheumatoid arthritis, the most common uses. There are also studies on the use of this medicine to fight AIDS, with results considered interesting but not definitive.
Three days after the release of the study, on March 21, Donald Trump, the US president, announced the discovery of Didier Raoult. He was responsible for putting the name of this drug on the agenda of all the newspapers in the world. Trump announced the possibility of a big "game change". The pandemic was already hitting the USA.
In early April, a doctor in a small town near New York announced he was already treating patients with this protocol. Dr Vladimir Zelenko, in addition to hydroxychloroquine and azithromycin, included zinc in the cocktail.
Zelenko, even being a simple doctor and not a scientist with a long history of research, apparently made a great discovery. All the information today suggests that the inclusion of zinc was an important evolution. Recent studies already link zinc deficiency with the severity of the disease.
At the beginning of April, Zelenko announced that he had treated about 200 patients, most of them elderly and other patients from risk groups. He reported that he did not have any deaths. Something very encouraging.
Claiming it is “anecdotal case” was the first argument against the use, but it was, in that brief period of time, a fair argument
The study from Marseille was only preliminary. They published the discovery despite being the result of only six patients with double therapy.
The study itself warned that it was preliminary. They published it quickly because the results were, according to them, very encouraging. They argued that the release occurred as a matter of ethics. They could not wait for a complete study, finalized, for publication. The news needed to be spread and lives needed to be saved from that moment on.
This is how we all learned what “anecdotal cases” are. What does that mean? That with few patients, without a more in-depth study, it cannot be considered scientific proof. It is needed to have more consistency.
Anecdotal cases are important in medicine because they suggest a treatment. From them, studies are developed, more complete, with a large number of patients.
Donald Trump announced with fuss. Anthony Fauci, the head of the U.S. task force in the fight against the pandemic, explained to everyone what the anecdotal cases are. He also detailed what the “gold standard” of science is, the maximum level of evidence: it is a placebo-controlled, double-blind, peer-reviewed, randomized clinical trial published in a prestigious medical journal with an impact factor.
According to Fauci, no medical treatment can prove its functioning if it is not a “gold standard” study.
What is a “gold standard” scientific study?
Randomized means to sort patients into two similar age groups, sex and previous diseases. In one of them, medication is applied. In the other, the placebos. The ones that receive the placebo are the control for comparing results.
Double blind means that neither the patients nor the doctors who are doing the treatment know which patients are receiving the placebo or the medicine.
Peer-reviewed means that, after the study is finished, before publication, other scientists check the scientific quality, do revisions and corrections. In other words, other scientists certify the quality of the study.
Scientific journals with impact factor are rankings created to designate the most important medical journals. It is a concept that seems to be interesting, but it is dangerous. Today the top three in the ranking are: the New England Journal of Medicine, the Lancet and Jama. There are several others. The bigger the ranking, the more prestige the published work has.
The acronym for randomized trials is RCT (Randomized Controlled Trial).
Before starting the randomized clinical trials to confirm or not the functioning of hydroxychloroquine, Raoult and Zelenko were mercilessly attacked
They went to investigate Didier Raoult’s life in detail. The story that most viralized was the one of a site with an imposing name: “For Better Science”. It is owned by the German Leonid Schneider. The first one came out a few days later, on March 26. In total, about Raoult, there were five articles. “Witchdoctor” was one of the titles. “Mad and dangerous,” concluded Leonid.
The dossier on the scientist’s life even addressed accusations of bullying and that he had covered up cases of sexual harassment that occurred at his institute. “End of the game?” asked one of the articles about Raoult.
Leonid also addressed some alarming cases, such as fakes that occurred in IHU-Marseille’s work. They found at least five works with changed microscope images in the photoshop.
The information that Raoul has already produced almost 3,000 articles, and that this would be statistically irrelevant, Leonid omitted.
I went to follow what Raoult was saying: he explained that one of the students modified these images and that this had gone unnoticed by the whole team.
Soon the article went in another direction, more bureaucratic. Raoult was charged with being a friend of the editor of the journal where the preliminary study was published. This discussion highlighted what I consider today a fetish among scientists with publications and with the “impact factor” of scientific journals.
I read carefully the article by Leonid Schneider. What promised to be a bombastic report, created a lot of expectation during the development of the text, but did not have the information about what I really wanted: and after all, the six patients were cured in five days or not? He did not answer.
“Miracle cure” was the way the New York Times referred to Raoult. All these stories served to assassinate the scientist’s reputation, but they are not at all important when compared to the death threats Didier began to receive shortly after proposing treatment with two generic and cheap drugs.
In the U.S., the main spokesperson for the treatment has become Dr Vladimir Zelenko. He published videos on Youtube saying that he treated patients with the medications. He stated that he obtained good results and that the immense majority of patients improved quickly.
Youtube deleted his videos for being “disinformation”. There is an imposed rule: you can only say that the drug works on social networks, science sites and big newspapers if there is a RCT (Randomized controlled trial) study with a positive result.
Shortly after, they did a report about Zelenko in the New York Times. They stuck on him the same “miracle cure” stamp they stuck on Raoult. The newspaper created a conspiracy theory: Zelenko’s motivation to claim that the drug was working could only be political, after all, Trump was enthusiastic about this treatment. Zelenko became a “Right-Wing Star”, wrote the journalists of the Times.
The story was a detailed profile of Zelenko. It explained that he had no sympathy for Hillary Clinton, that he lived in the countryside, that he was recovering from cancer, but failed to investigate the only thing that really mattered: and after all, his patients, did they or did they not die?
Because if he treated 200 high-risk patients and nobody died, it would be the scientific proof of the functioning.
It’s that simple. It is the most basic rule of science: reproduction.
It’s really simple. The disease has a start, middle and fast end. In about 15 days after the symptoms are present, without any effective medication, a percentage between 3 and 6% of symptomatic patients need to be intubated to stay alive.
In this expectation, at least six patients should have died. Any number below that, in a normal distribution of American society, means that the drug worked.
And then a fork occurred between real life science and the science of scientific bureaucracy
With the information that medical recommendations can only be made with positive randomized trials (RCT), the “scientific method” was followed.
They went to produce RCT studies, to be peer-reviewed and then published in impact journals.
In addition, RCT studies are time-consuming, very expensive, take time to design, organize and present the results.
In this context, all science journalists began to write and explain what randomized, double blind, peer-reviewed studies are. And government decisions, from the WHO (World Health Organization) and the FDA, a U.S. agency, kept waiting for the randomized and controlled studies.
On the other hand, in real life science, with the good evidence of Didier Raoult’s first study and the confirmation by Zelenko, doctors began to treat patients with these drugs. Thus other types of studies began to be produced: the observational studies. It’ s faster and cheaper to make.
What are observational studies and what are the differences between them and RCTs?
Doctors, clinics or a hospital treating patients in the mid-pandemic can do observational studies with a certain degree of ease. They can either confirm an existing protocol, such as that of the IHU-Marseille, or they can include more drugs.
The difference between observational and RCT is that there is no placebo randomization and double blind control. Doctors know they are delivering the medications and patients know they are taking the medications.
The comparison, to know if the treatment was successful or not, is with non-medicated patients. These patients may be from the same hospitals, from other hospitals, or with an overall average mortality rate in the city, region or country.
And because of the lack of randomization, i.e the similar distribution of patients by characteristics, among those receiving the drug or the placebo, if the difference in clinical results between the groups is small, it is more difficult to judge whether the treatment worked or not.
The four possible kinds of hydroxychloroquine use against COVID-19
There are four possible uses of hydroxychloroquine. What Raoult proposed was early treatment. That is, the beginning of treatment in the first days of symptom, before the disease gets worse. This is the most obvious use. In every disease the doctors recommend starting the treatments as early as possible.
In addition, there are other possibilities. The first is the pre-exposure prophylaxis: this is when patients take the medication before having contact with the virus.
The second is post-exposure prophylaxis, which is when the patient takes the medication just after having contact with someone infected, and the third possibility is treatment already with the advanced disease, severe, in patients already hospitalized, needing oxygen or intubated.
In real life science, observational studies with hydroxychloroquine in early treatment shows spectacular results
There are several observational studies, besides those done in the IHU-Marseille, of treatment with the HCQ + AZ protocol in the first days of symptom. There are some in monotherapy and some with other combinations of medication. Here I bring some that made clear in their studies that it was an early treatment.
Timeline of observational studies in early treatment:
May 22nd
Retirement homes in New York, USA
Instead of the combination of hydroxychloroquine and azithromycin, the second drug was doxycycline. The study led by Imtiaz Ahmad was conducted with 54 high-risk patients in three nursing homes in New York. Only 11% of patients were transferred to hospitals and only 6% died.
The comparison was with another nursing home. In King County, Washington, where there was no treatment, 57% of patients were hospitalized and 22% died. “Decreased transfer to hospital and decreased mortality were observed after treatment”, said the scientists.
It’s a huge difference, how can we say it doesn’t work?
May 31st
Private clinics in France
In an study done by Violaine Guérin and her team, the results of 88 patients were followed. The combination of hydroxychloroquine and azithromycin reduced deaths by 43% and recovery time by 65%, compared to the control group.
June 25th
IHU-Mediterranée Infection, Marseille, France.
The institute where Didier Raoult is professor published his “final”, more solid study with 3737 patients. Earlier they had published two previous ones, with 80 and with 1000 patients.
From the total, 3,119 received the combination of drugs. The mortality rate was 0.5%. The most impressive result is that no person under 60 years of age died, and a good part of the total had previous comorbidities: 7.5% had diabetes, 13.1% hypertension, and 11.1% was obese.
People can criticize this observational study as much as they want, but one fact is unchangeable: no one under 60 died. This is an impressive fact.
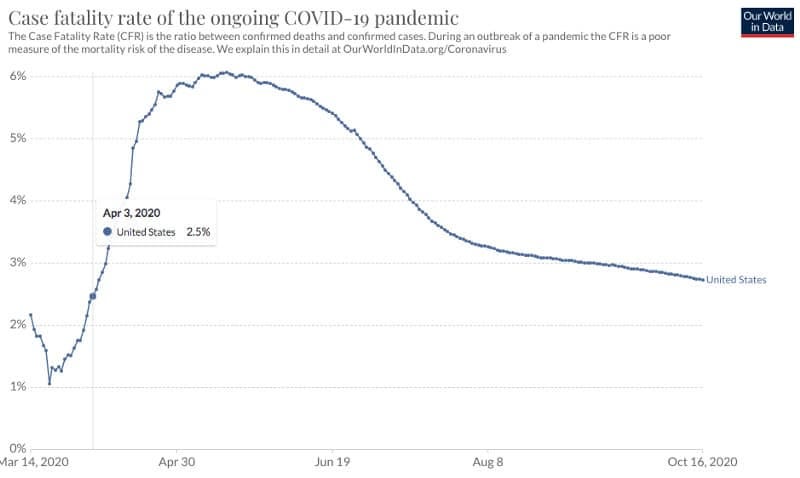
For comparison, in the region of Ile-de France, where Paris is located, no medication was used. The deaths there, under 60, were little more than 9.7% among the fatalities. In another region of France, the Grand-Est, 4.3% of the deaths represented the population under 60.
In another public hospital in Marseille, about 2.5% of the infected died. Among the patients who knocked on the door of the IHU-Mediteranée Infection, only 0.5% died.
It is a brutal difference. How does it not work?
August 13th
Saudi Arabia
The study was conducted by Tarek Sulaiman’s team from King Fahad Medical City, Riyadh, Saudi Arabia, and involved 7,892 patients treated in 238 clinics throughout the country. 3,320 patients received hydroxychloroquine, and the comparison was with 5,572 who did not had the medication.
It involved patients only with a positive test. Among those who took the medication, more than 70% in the reduction of mortality. “Early intervention with HCQ-based therapy in patients with mild to moderate symptoms at presentation is associated with lower adverse clinical outcomes among COVID-19 patients” concluded the scientists.
August 21st
Nursing homes in Marseille, France
Done by Dr Tran Duc Anh Ly and his team, the study involved patients with an average age of 83 years. There were 226 infected residents, 116 treated with hydroxychloroquine and azithromycin. 53.5% fewer deaths among those who took the medications.
August 25th
Hackensack University, USA
The study by Andrew Ip, from Hackensack University in New York, involved 1,274 patients. It was only with hydroxychloroquine, without azithromycin, and 97 took the medication. The comparison was with 1177 patients who did not take it. The early treatment was associated with a 47% reduction in the risk of hospitalization, concluded the scientists.
September 2nd
Nursing homes in Andorra, Europe
Coordinated by Dr. Eva Heras, the study occurred only among the elderly. It involved 100 patients and the average age was 85 years. Among the patients who received HCQ and Azithromycin, 11.4% died. Among those who did not receive the drugs, 61% died.
October 31st
Study by Dr Vladimir Zelenko, from USA
Zelenko teamed up with Roland Derwand and Martin Scholz, two German researchers, to produce a study and publish it. It is about his patients treated near New York.
In besides the addition of zinc, there is a difference between his protocol. Zelenko did not treat patients who were not in the risk group. In other words, the drugs were prescribed only for those over 60 or, if under 60, with at least some comorbidity.
The study included 144 patients with an average age of 58 years. As a control group, 377 other patients from the same community. Among those who received the medication, only one died (0.7%), among those who did not, 13 died (3.5%).
How does it not work?
October 31st
Hapvida Health Care Provider, Brazil
The Hapvida company is one of the largest in Brazil. It has millions of clients. The study involved 717 outpatients who were positive for SARS-CoV-2. All with 40 years or more. It was done by Brazilian researchers from Hapvida, the Federal University of Fortaleza and Professor Harvey Risch from Yale.
Among those who did not take hydroxychloroquine, 3.3% of deaths. Among those who took the medication, and in most of them together with azithromycin, the number of deaths was 0.6%. “This work adds to the growing literature of studies that have found substantial benefit for use of HCQ combined with other agents in the early outpatient treatment of COVID-19”, concluded the scientists.
Today, the day I am writing, December 2nd, there are 23 studies in early treatment with hydroxichloroquine. All, without exception, with positive results for the patients. Check all of them in this link.
A simple digest of observational studies in early treatment: among patients who took medication, less deaths
To have a look at all these results and say that the drug is not scientifically proven is similar to calling all these scientists imbeciles. It is hard to do.
Think along with me.
Scientists provide the medication, and they find that among those who took it, fewer patients died. And the scientists highlight this in their studies. The connection with the smallest number of deaths, of course, is with medication.
So you say it’s not scientifically proven. And that among those who took hydroxychloroquine, fewer patients actually died, but not because of the drug, but for some other random reason.
This in every early treatment study!
I don’t need to be a scientist, with a PhD in medicine or microbiology, to get angry with people who believe they are smart, intelligent and that all other people are morons. That is to go beyond the reasonable limit of civility.
Think about the following dialogue with a person who denies the functioning:
- In this study here, from France, there were 53.5% fewer deaths among those who took hydroxychloroquine.
- But the drug does not work, it is not scientifically proven.
- Are you saying that those who took it died less, but for another reason, is that it?
- Exactly.
- But why did they die less?
- I don’t know.
- I do not know. It’s okay. There’s this other study here, from the U.S., only with old people. The scientists said that among those who took it, 6% died, and among those who didn’t, 11% died, but it’s not scientifically proven, right?
- That’s right. The drug doesn’t work.
- So among those who took hydroxychloroquine less died, but for some other reason, is that it?
- Exactly.
- And Didier Raoult, what do you think of him?
- Fraudator
- And Zelenko?
- Trump supporter.
- What about the scientists from Andorra, Brazil and Saudi Arabia, all fraudsters and defenders of Trump too?
- Probably.
- And you, how do you define yourself, a defender of science?
- Exactly.
- What is your religion?
- I am a faithful devotee of the fundamentalist church of the randomized, controlled and double blind.
I am not a scientist. I think in a very simple way, but I think this is a conversation of those who need a straitjacket.
And science confirms that it is, yes, talk from those who need a straitjacket
In this pandemic there is a dogmatic definition: hydroxychloroquine can only be recommended by governments and organizations if we have a placebo-controlled RCT demonstrating positive results.
The other definition is that you can only say that the drug works, both on social networks and in newspapers, if you have a positive RCT. Anything other than that is “disinformation” and needs to be censored.
Furthermore, it is authorized to insult doctors who prescribe drugs without RCT. They are quacks, deceivers, conspiracy theorists and “anti-science”.
That’s probably how medical science has always worked, right?
No. It’s a fake speech.
The history of medical science is based on observational studies, but there has been a convenient change in the rule right now, in 2020, during this pandemic, right at the moment the world is in a hurry.
In a 2011 a scientific study by Dong Heun Lee showed that only 14% of the Infectious Diseases Society of America’s treatment guidelines were based on the “highest level” of evidence, the requirement they want from hydroxichloroquine.
When we talk about cardiology medicines, 89% of the recommendations do not have this evidence.
Have you ever seen a doctor who prescribes insulin for diabetics called an “anti-science” or a quack? They should be called that, because there has never been a “gold standard” study on insulin.
Have you ever been vaccinated against tetanus? It also does not have the “highest level” of evidence. Should we say that this vaccine was made without scientific basis? The theorists of the anti-vaccine conspiracy would go to the delirium.
It was never done for insulin or tetanus vaccine because it is not necessary. In a 2014 scientific paper, Andrew Anglemeyer, an epidemiologist at the University of Otago, New Zealand, explained that there are no significant differences in results between observational studies and the “gold standard”. In another study, published in 2000, Kjell Benson came to the same conclusions.
In other words, historically, the results shown by the observational studies match the “gold standard”.
Moreover, before the pandemic, science used to say something else. Angus Deaton, a scientist at Princeton University, USA, in 2018, explained that the gold standard is not as “gold” as they say. “RCT results can serve science but are weak ground for inferring ‘what works’”, he explained.
In a 2017 article, the scientist Thomas Frieden, appointed director of the U.S. CDC by Barack Obama, argued in his scientific article, published in the New England Journal of Medicine, that public decisions on treatment should not be based on RCTs.
Frieden commented on the “increasing costs” of “gold standard” studies, in addition to the delay in carrying out such research. “These limitations also affect the use of RCTs for urgent health issues, such as infectious disease outbreaks,” he wrote.
In recent years, just before COVID-19, medical science seemed quite reasonable, didn’t it?
How did the mainstream media handle the observational studies?
After Didier and Zelenko, as it was difficult to call all the authors of all these studies crazy, “miracle healers” radicals of the far right and fraudsters, the solution found by the media and scientific communicators was the silence. No news were published about the observational studies of early treatment.
The New York Times, for example, only reported twice on the observational studies. One which was later retracted by the Lancet for containing fraudulent data and another made in Brazil with a dose of 1.2 grams per day for 10 days, four times the dose proposed by Didier Raoult, and only in severe patients with the advanced disease.
Before we continue, a short story about AIDS between 1987 and 89
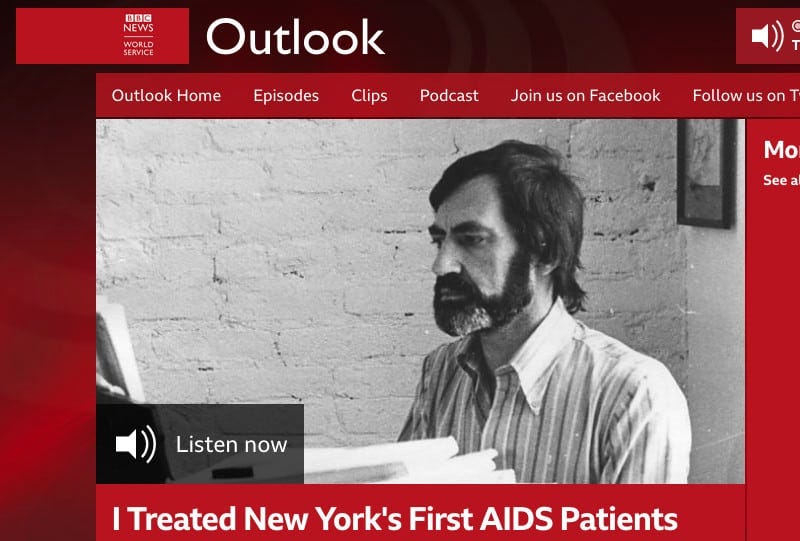
In 1987 a tense meeting took place. Present were AIDS activist Michael Callen, Dr Barry Gingell and Dr Anthony Fauci, the Federal Tsar on AIDS in the USA. Michael and Barry begged Fauci to help promote the use of the drug Bactrim as a prophylaxis for pneumonia caused by the disease.
The HIV pandemic was killing a lot. The world was scared and there was intense media interest. The two men explained to Fauci that front-line doctors, following the protocol of Joseph Sonnabend, a South African scientist, were using Bactrim very effectively, with a high percentage of success.
All scientific evidence of the drug’s functioning was refused by Fauci. Sonnabend was seen as controversial, polemical, and as someone who was attacking science. There was no “gold standard” study of Bactrim. At the same time, no one was in a hurry to conduct such a clinical trial.
It was a strange reaction, because some years before, when Dr. Fauci was studying another disease, Wegener’s Granulomatosis, he developed a treatment with only 18 patients. It was a purely anecdotal study, with no controls and no placebo. The results were compared only with historical data and his therapy became the standard of care, without encountering any barriers.
While this discussion continued, Bactrim’s competitor, the lucrative AZT, from a large pharmaceutical industry, with little efficiency and strong side effects at a cost of US$ 8,000 per year per patient, was approved in a record time of only 20 months. It was a reutilization. AZT was originally thought to be a cancer drug during the 1960s, but was archived when it was found not to be effective enough.
It was only two years later, in 1989, that evidence of cheap Bactrim was accepted and the recommendation happened. During this period, 17 thousand lives were lost.
Sean Strub tells part of this story in a report in the Huffington Post. This horror is well documented and told in several books and reports.
As this medical scandal occurred in people with AIDS, mainly affecting the homosexual community, a large part of the population understood these deaths as divine punishment for sinners. History has been forgotten, lessons have not been learned and no reform in medical science has been made.
Gilead’s Remdesivir easy path to the “gold standard”
Remdesivir, a competitor of hydroxychloroquine, was developed for Ebola. It did not achieve much success in its initial mission and was reused for COVID-19.
The manufacturer is Gilead, a pharmaceutical giant with 11 thousand employees and a monstrous revenue of US$ 22 billion.
In the first quarter of 2020, as the name of the drug gained notoriety during the pandemic, Gilead increased its spending on lobbying the administration and the U.S. Congress.
With a manufacturing cost of about $10, Remdesivir costs $3,000 per patient to treat COVID-19.
Being a “gold standard” drug, Remdesivir started directly with the expensive “gold standard” trial.
However, as the Washington Post reported, this study had, during the clinical trial, a change in metrics from mortality to recovery time. The drug did not reduce deaths, but only reduced the recovery time of those who would not die, from 15 days to 10 days.
And although failing to reduce mortality but having an RCT study, the U.S. government, on April 29, announced Remdesivir as the “standard of care”.
Gilead then signed a US$ 1.2 bi agreement with the US government to supply the medication. Soon the company made another deal, this time with the European Union, of US$ 1.0 bi. At the same time, Gilead was paying a $97 million fine to the U.S. Department of Justice for allegedly paying illegal bribes.
In addition, while several news reports bombard us about the very strong side effects of hydroxychloroquine, which is false according to several studies, Remdesivir, which has been seriously compromising the kidneys of patients treated with this drug, leaving many of those who survived on dialysis machines, is not receiving the same media attention regarding the side effects.
And instead of reporting patients on dialysis machines, the New England Journal of Medicine, the world’s leading medical journal, took a friendly approach and published an editorial about the medicine: “Remdesivir — An Important First Step,” the title said.
On the difficult path of hydroxychloroquine to the “gold standard”, a porn actress enters the scene. And the world preferred to trust in her.
On May 22, a study about hydroxychloroquine was published in the Lancet, the second most prestigious medical journal in the world. The main name was Dr. Mandeep Mehra, professor of medicine at Harvard, USA. The research reported that he used data from 96,000 patients in 671 hospitals worldwide.
It concluded that hydroxychloroquine, promoted by Donald Trump, increased the risk of death. In addition, that the drug produced dangerous cardiac arrhythmia. There was a coincidence: the result matched like a symphony in the narrative of the mainstream media about the dangers of the medicine.
This study has become headline news in every major newspaper in the world, along with criticism of Trump, the U.S. President, for being anti-science and bringing risks to Americans for promoting this drug.
On May 25, WHO (World Health Organization), based on these results, interrupted their "gold standard" study on hydroxichloroquine. The Guardian, one of the most important newspapers in Europe, in addition to reporting the cessation of clinical trials, qualified Professor Didier Raoult as “controversial”.
Several other “ gold standard “ worldwide were also interrupted due to the Lancet study. Among them, Hycovid and Discovery, both in France. And an important detail: the partial results of both showed positive results for the patients who took the drugs, compared with the placebo, when the studies were interrupted.
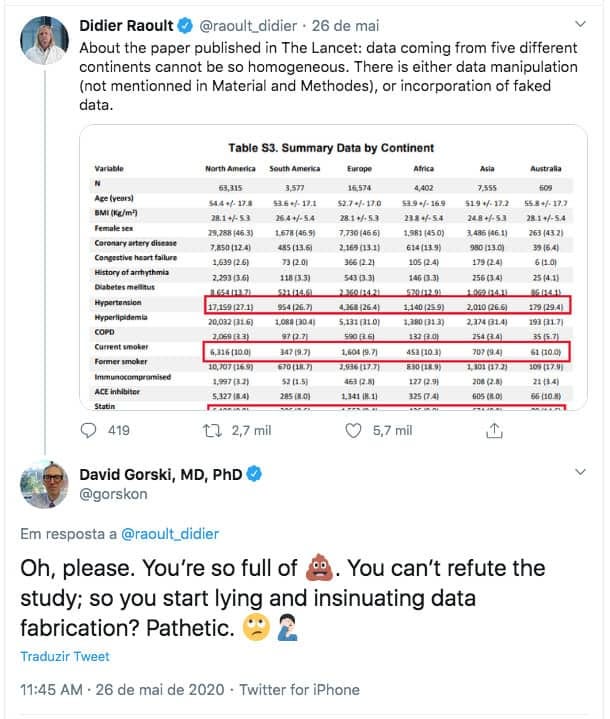
Four days after the publication, on May 26th, the experienced professor Didier Raoult went to his Twitter and made a bombshell accusation: he said that the data from the Lancet study were manipulated or falsified.
It is certainly an accusation of those who need to be very sure before making it. He simply said that one of the most prestigious medical journals in the world published a fake study, and from a professor at Harvard, one of the most important universities in the world.
With an accusation of this level, either the data were really false, or Raoult’s career would be over at that moment. It was a tense moment in science.
With the favorable atmosphere to call charlatan, forger and censor anyone who says hydroxychloroquine works, David Gorski, professor of medicine, researcher, and who proudly boasts the position of editor of the website sciencebasedmedicine.com, where he proposes to teach the world what is medicine based on good science, decided to offend Raoult at the same time.
In addition to placing, without any embarrassment, a faecal icon to refer to Raoult, Gorski called him a liar and pathetic.
Then serious scientists mobilized on the alert raised by Raoult. They went to research where the data came from. The origin was an obscure company called Surgisphere. Among the data used to produce the study were nonexistent hospitals. One of the main employees of Surgisphere was a porn actress.
It’s one of the most pornographic scandals of science until the moment. With these data discovered, finally the backstage stories with hydroxychloroquine started to be published in the mainstream media.
In the end, the Lancet study, which involved a porn actress and a renowned Harvard professor, after immense pressure from the scientific community, was retracted less than two weeks after it was published. Didier Raoult was right.
“There are people who have tried and succeeded in making governments and the WHO believe that a medicine that is 70 years old, one of the two most prescribed drugs in humanity, have killed 10% of the people it was given to,” Raoult commented recently in an interview.
“It is something that should lead us to reflect on the state of our society, which can be deceived in an incredible way,” said the professor.
Still on the case, two curiosities: the first is that David Gorski still hasn’t apologized to Raoult. The second is that unlike the videos of Frontline Doctors, U.S. doctors who reported good results with hydroxichloroquine and were censored on YouTube for “misinformation,” the interviews of Mandeep, the author of the study with fake data published in the Lancet, talking about pornography on hydroxichloroquine, are still on air, available on YouTube.
In the bumpy path of hydroxychloroquine to the “gold standard”, another controversial study was published by NEJM
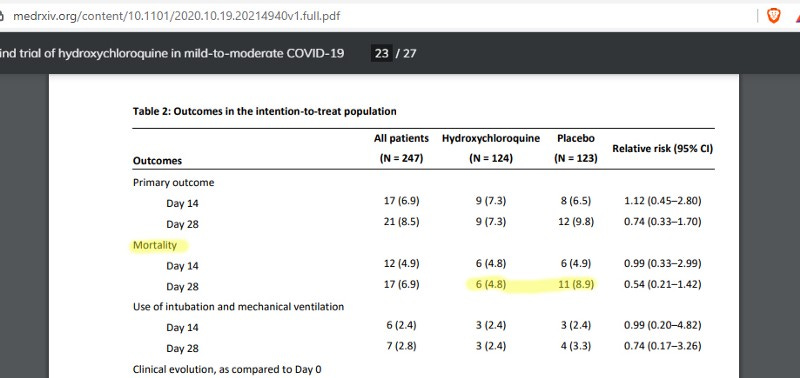
On June 2, 2020, two days before the Lancet farce came to light, a “gold standard” study was published in NEJM (New England Journal of Medicine), the largest impact factor in the world. It was originally thought to involve 1300 patients, but had just over 800.
Originally from the University of Minnesota, USA, led by David Boulware, it was about post-exposure prophylaxis. It is when the medication is given to people who had recent contact with someone contaminated. It is already one of the most controversial studies in the history of medicine.
The data from the study were presented as follows: although they showed positive results for those who took the hydroxychloroquine, they were only very modest and statistically insignificant results, that is, they could have occurred at random.
It represented the definitive burial of hydroxichloroquine. It is the study that most viralised in the medical world as definitive proof that the drug does not work. In any debate people sent this link.
After all, it was a randomized, double-blind, placebo-controlled study and published in the world’s most respected medical journal.
The argument was that a “gold standard” study, for being a higher level of evidence, would invalidate the positive results of the observational studies.
Several controversies, which last until today, have occurred about this study. While the observational study, conducted in São Paulo by the Prevent Senior Health Care Operator, with positive results for hydroxychloroquine, was rejected by the medical community because the patients’ diagnosis was not due to COVID-19 tests, but by symptoms, the University of Minnesota study, also deficient in tests, but without positive results, was celebrated, without any criticism, by a large part of the medical and scientific community.
Believe me, the method of the study was an internet survey. They mailed the medications and placebos, and people returned their symptoms on forms. A less accurate process than Prevent Senior's, where they sent the medications by courier to the patients' homes and checked the symptoms by telemedicine on video, in interviews with the patients, or by advanced lung injury exams. Moreover, in the case of São Paulo, if the patients worsened, they would be admitted to the operator's own hospital, with more ease to follow the outcomes. In contrast, the virtue of Boulware's study was to be randomized.
This study by Boulware, for having become a reference, generated heavy complaints from Raoult’s team. They sent an Expression of Concern to the publisher. They concluded: “NEJM, How long will you abuse of our patience? The biases shown in the studies on the COVID-19 have gone beyond, as in the Lancet for that matter, everything that has been seen so far. Please give us back a journal that we can use for medical education that does not contradict all principles we have used for so many years”.
The difference in approach can also be compared with the case of Remdesivir’s approval. In the case of the Gilead drug, the study that was used for its approval by the FDA showed modest results and not statistically significant, but this did not stop the approval, generating movement in the stock markets.
But Boulware’s study, in fact, scientifically confirms the functioning of hydroxychloroquine
Everybody is staying home a lot, afraid, avoiding to go out as much as possible and practicing social distancing. However, the pandemic has arrived for everyone and something new is happening in science: a large number of people have started to study scientific publications.
Before, the studies of medicines were very restricted in small groups of researchers and medical newspapers. Today a large number of scientists from various fields are checking all the publications in details.
The peer review process is undoubtedly one of the most important values of science. Thus many scientists, seeing hydroxychloroquine being denied to the population, and amazed that the drug showed significant results in observational studies and not showing the same performance in “gold standard” studies, contrary to the logic and history of medicine, decided to go deep in exactly the point that was blocking: the randomized, double blind and placebo controlled studies. In other words, these scientists went to play in the opponent’s field.
Marcio Watanabe, professor of statistics at the Universidade Federal Fluminense and PhD in statistics at USP, one of the most prestigious universities in Latin America, was one of the scientists who reviewed Boulware’s work at NEJM.
With an in-depth analysis, he found that the patients who received the drug earlier had greater effects. Boulware’s study was misinterpreting its own data and presenting it in the wrong way. When it takes a long time for prophylaxis and mixes all patients over time, the effect loses statistical potency.
When the data are analyzed taking into account the interval between exposure and the beginning of treatment, they reveal a clear pattern: patients who started treatment earlier had better results than those who started treatment later.
The data indicate that taking the hydroxychloroquine right on the day of exposure could lead to a reduction of symptomatic contagion of more than 50%, Watanabe concluded. Short times in post-exposure prophylaxis is normal in medical science. In cases of exposure to the AIDS virus, prophylactic treatments, to have effects, involve a few hours, not days.
I interviewed Watanabe to know what the outcome of his review sent to NEJM. “I never had a response from NEJM, neither negative nor positive. They said they would only analyze the letter at a future moment, without giving a date”, said the professor from Rio de Janeiro.
The mistake in Boulware’s conclusion is so evident that other scientists have done practically the same analysis.
A group led by David Wiseman, a scientist from Dallas, together with four other U.S. scientists, including some from the Henry Ford center of medical excellence, produced a second review on the same NEJM study. They reached numbers similar to Watanabe.
In a third review, Juan Luco, professor at the Universidad Nacional de San Luis in Argentina, also analyzed the raw data and arrived in statistically significant numbers. “It shows that the published conclusion of the group that HCQ does not prevent COVID type infective symptoms was fundamentally flawed and should be reconsidered.” he said in the study.
I asked Juan if he sent his review to NEJM. “I did not send anything to the NEJM. It is impossible to expect honesty and scientific truth from them about hydroxychloroquine,” he answered.
In a fourth review, six more scientists led by Alexander Chuan Yang, from Wayne State University School of Medicine, reached the same conclusions: “However, our re-analysis of the data suggests HCQ use for Covid-19 is time-sensitive”, they stated.
In a fifth review, the mathematician Phill Birnbaum, from Sabermetric Research, posted in his blog the study’s failed interpretation. “In other words: they stopped the study just as the results were starting to show up”.
That is, we have several important scientists who looked at the data, analyzed, wrote, put their names and reputations at stake and concluded that Boulware’s study shows wrong results.
Boulware’s study, as it stands, is positive within the margin of error. And with the correct analysis, it becomes positive outside the margin of error. But all revisions were ignored.
And what is known so far is that no one has been able to explain, by mathematics, that these revisions are wrong.
In other words: this is the scientific proof of the functioning of hydroxychloroquine in a “gold standard” study.
And another thing that is known is that it would not make sense for all these scientists of these reviews to be in a big corrupt global conspiracy to promote hydroxichloroquine. After all, it is a generic drug, cheap, without patents and manufactured by hundreds of laboratories around the world.
The question that remains on this case is: why NEJM ignored all these reviews that change the result?
And there is a second question: why is the mainstream media not reporting on this issue and demanding an answer from NEJM?
Before we continue, a brief explanation about statistical significance
People living in democracies have an easy understanding of what statistical significance is when hearing news about election polls.
“Candidate Joseph is leading with 46% of voting intentions. In second place is candidate John with 40%. They are tied within the 3% margin of error. 1200 voters were interviewed,” the news says.
Statistical significance relates to the margin of error. In other words, even with Joseph leading, there is a small possibility that they are tied with 43% each and the result was by chance.
But if the survey had been done 2 or 3 thousand voters, instead of 1200, the error margin would be smaller, 1% or 2%. In this case, the candidate Joseph would really be leading, and thus would be reported. The chance of being a by chance result would be much smaller.
Now follow me. On the same day another electoral survey with similar results comes out. Joseph is with 46% and John with 40%. Also with a margin of error of 3% and 1200 voters interviewed.
From that moment on, Joseph is really leading. The two surveys put him in the front. It’s no longer by chance, because the margin of error has reduced in a combined statistic.
That is, we have two surveys “within the margin of error”, but when combined, the margin of error has reduced. Joseph is no longer leading “ by chance”.
In medical research the principle is the same. Marcio Watanabe made some example calculations. One of the “scientifically proven” drugs was Dexamethasone. It reduced deaths by 30%. Dexamethasone works only for critically ill patients, intubated or in oxygen support.
The study had more than 2 thousand patients. If it had been done with the number of patients similar to the University of Minnesota study with hydroxychloroquine, with 821 patients, Dexamethasone would not be “scientifically proven”. And any doctor who speaks of this drug would, of course, be a quack.
All “gold standard” studies of hydroxychloroquine, in pre-exposure, post-exposure and early treatment prophylaxis, bring positive results to patients. It is scientific evidence at the highest level of scientific evidence
“It is increasingly difficult for them to say that hydroxychloroquine does not work”, Flavio Abdenur told me. One more “gold standard” study had just come out when he sent me this message.
Flavio is a mathematician. He has a doctorate from the Institute of Pure and Applied Mathematics (IMPA), was a university professor and today works with statistical analysis of data in the private sector. He is part of a group of virtuous Brazilians of which Watanabe is part. This group includes doctors, biologists, virologists, economists, mathematicians and statisticians.
They decided to study treatment options in depth. Flavio showed interest in studying the subject out of concern. “My parents are in the risk group,” he said.
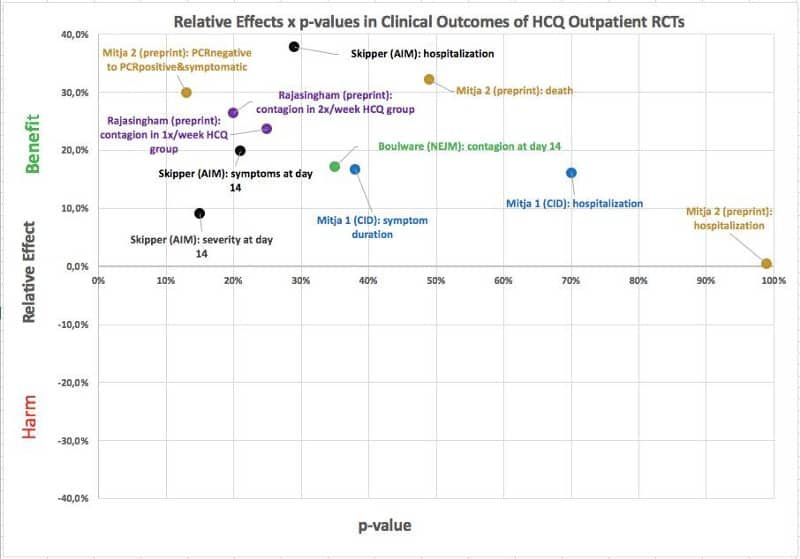
Flavio assembled this graphic and published it on his facebook. Being transparent, he also made available the file with all the data for those who are interested in going deeper.
At the top, studies that show positive results to patients. At the bottom, the ones that show negative results. None shows a negative result. They all show positive results.
Yes that’s right. In all “gold standard” studies, patients who received hydroxychloroquine had a better result compared to the placebo group.
But all of them, isolated by statistics, show a “tie within the margin of error” because they are few patients. Even with some benefits being of high values, such as the 37% reduction in hospitalization needs of the Skipper study. Or like the 30% death reduction in the Mitja study. This is because all these randomized are quite small. Its groups have at most a few hundred patients each. In the jargon of the area, they are statistically “underpowered” studies.
And when combined, they leave this margin. That is, the hydroxychloroquine is the coin that when thrown up always falls on the same side. Always. There is no longer the possibility of the results being “ by chance”.
“Remembering that these randomized studies used only HCQ. A long and growing series of observational studies indicates that, in combination with other medications, the effect is stronger, as long as they are used right at the beginning of the symptoms,” said Flavio.
One more analogy for everyone to understand: a race with two cars was organized. The hydroxychloroquine car and the placebo car. The winner is declared only after the car that leads complete 50 km.
The race had five starts. But the judge stopped all five after 10 km driven. But in all of them, when the interruption occurred, the hydroxichloroquine car was leading.
When you add the five races, the hydroxychloroquine car completed the 50 km in the lead.
The earth is not flat
It is simple. For someone to look at Flavio’s graph and find an explanation to say that hydroxychloroquine does not work, it is necessary to be as creative as the people who look at the picture of our planet and find a way to continue saying that the earth is flat.
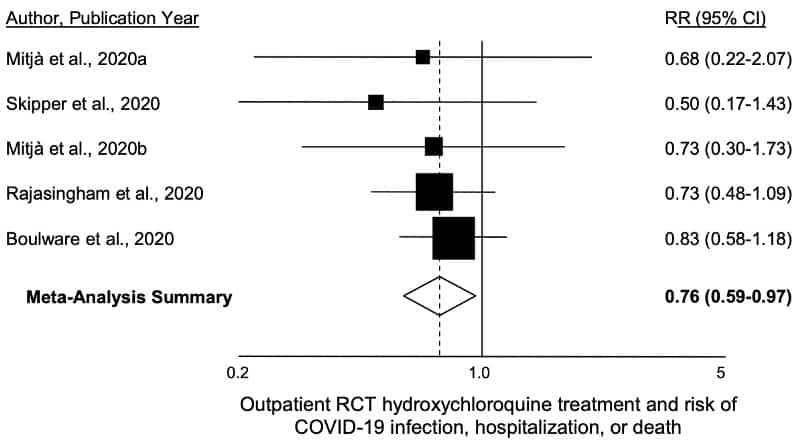
Professor Harvey Risch from Yale made a meta-analysis with the same principle
The joining of studies for a general analysis is called meta-analysis. It is the highest level of scientific evidence. The award-winning professor Harvey Risch from Yale, one of the most important universities in the world, together with two other renowned professors, has produced a study with the same principle. These scientists went further than Flavio and did all the math, not just a graphic explanation.
It is also based only on “gold standard” studies. Objective? To eliminate the last argument of those who deny the functioning of medication.
The list of all studies is on the left, indicating benefits for those who have taken the medication. When combined, the margin of error disappears.
And a curiosity: this meta-analysis of professor Harvey Risch viralized in the social networks of Brazil. This was the trigger for Brazilian “fact-checking agencies” to expose their entire arsenal of infinite stupidity and demonstrate that they dare to argue what they don’t understand.
Lupa Agency wrote: “No double-blind, randomized study has so far proven the efficacy of the drug as prophylaxis or treatment in early stages of the disease. On the contrary: a study published in the Annals of Internal Medicine, and cited in that meta-analysis, demonstrated that the drug is ineffective for the treatment of non-hospitalized people”.
Another agency, called “To the facts”, showed the same ignorance when talking about the studies used in meta-analysis. “All five have conclusions that go against the efficacy of chloroquine,” they said.
Yes, it is true. No study alone demonstrates efficacy beyond the margin of error, but when combined, the number of patients increases and the studies begin to demonstrate efficacy.
The agency’s statement also linked to an opinion piece by Carlos Orsi, a science fiction writer. And by the miracles that the Internet age generates, this writer feels qualified enough to say that meta-analysis is wrong. In the text, Orsi called scientists and doctors charlatans.
“It’s a pathetic text that shows that the author has no idea what a p-value or meta-analysis is,” said Daniel Tausk, professor of mathematics at USP, one of the most prestigious universities in Latin America.
“It seems that they are people who are used to some rather trivial debates against some bizarre pseudosciences and ended up extrapolating the aggressive attitude to complicated things, out of the scope of what they can evaluate,” he added.
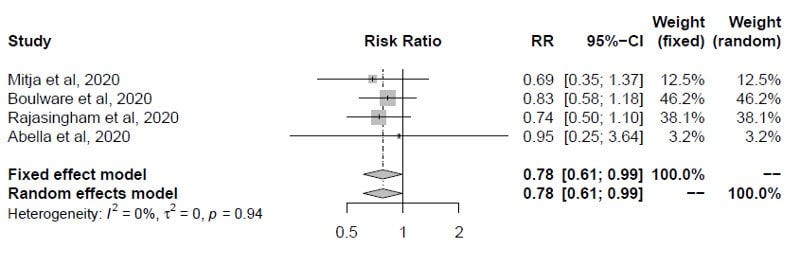
Harvard professor made a similar meta-analysis, only about prophylaxis
Miguel Hernan, professor at Harvard, together with three other Spanish scientists, produced another meta-analysis on the same principle of joining the studies of Harvey Risch and Flavio Abdenur. This one is about the randomized HCQ as prophylaxis. It also found a positive and statistically significant result for the clinical effects.
This study, as it did not viralize, did not become a target of the “fact checkers”.
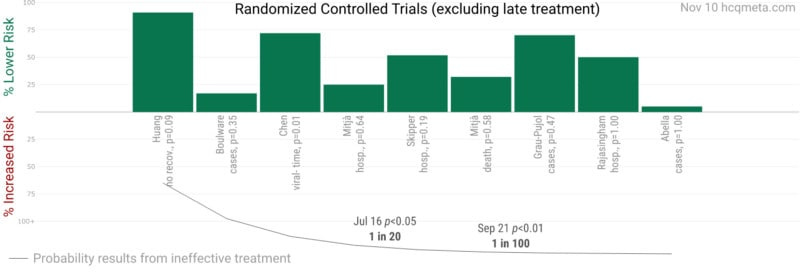
A third meta-analysis, using the same principle, draws the same conclusions
A group of scientists who preferred to produce in anonymity, due to the various numbers of layoffs, attacks on reputations and possible future budget cuts, produced a meta-analysis in which one of the points focuses only on randomized, double-blind, placebo-controlled papers.
Including only the “gold standard” studies in prophylaxis and early treatment, the chance of being “the work of chance” is only one in 100, they concluded.
For comparison, the “scientifically proven” standard of medicine is if the chance of being at chance is one in twenty. This barrier has been broken several times.
In the graph, the same concept: all studies show positive results. None shows negative results.
None of these meta-analyses are peer-reviewed or published in any “impact factor” journal. Apparently, nobody wants to publish. It’s an incendiary subject. But from the moment you have four distinct groups doing the same statistic, with practically the same method, and arriving at the same result, one study represents the revision of the other.
No one has appeared, nor will they appear, explaining that these calculations are wrong. It’s mathematics and statistics. You can’t shout against numbers.
Therefore, anyone who denies these meta-analyses is a denialist of science.
Suddenly, scientists who did not pay attention to the statistical significance of the studies began to talk about this, but about the masks
Recently a study was published on the effect of masks to prevent the contagion of the coronavirus. It is from scientists from Denmark. It is a randomized study. 3,030 people were assigned to wear the masks, another 2,994 people were the control group.
The result of the study is statistically inconclusive: by itself, it is not enough to show that the use of the masks brings significant benefit to avoid contagion. Among those who used them, 1.8% were infected. Among those who did not wear, 2.1% was infected, but the probability of the result being at chance is big.
Eric Topol is a doctor, scientist and editor-in-chief of Medscape, one of the most important medical websites in the world. He has always set himself against hydroxychloroquine. Several times.
With the study of masks not pointing out scientifically the benefits, he should put himself against the use of them by the population, as he did with the randomized studies of hydroxichloroquine.
Suddenly, Topol analyzed that a study with few patients do not bring positive results, but apparently, he is only able to do this analysis on masks. “Underpowered,” he said.
And the sensible thing, with these results, is not to start a war to prohibit the use of masks by the population, but to wait for more studies with more patients. Probably it should have positive results. About 15 to 20% in the reduction of contagion.













SO well written! Thank you for a comprehensive review of the science that should have resulted in HCQ, zinc and AZ pack becoming a widespread early treatment. It's incomprehensible that the naked greed of Pfizer et al has allowed suffering and death on such a massive scale. Same has happened with ivermectin.
Hi, excellent, important work. Just for your information, there is a mistake, you incorrectly calculated the numbers :) or the number of patients was incorrect -
The study was conducted by Tarek Sulaiman’s team from King Fahad Medical City, Riyadh, Saudi Arabia, and involved 7,892 patients treated in 238 clinics throughout the country. 3,320 patients received hydroxychloroquine, and the comparison was with 5,572 who did not had the medication.